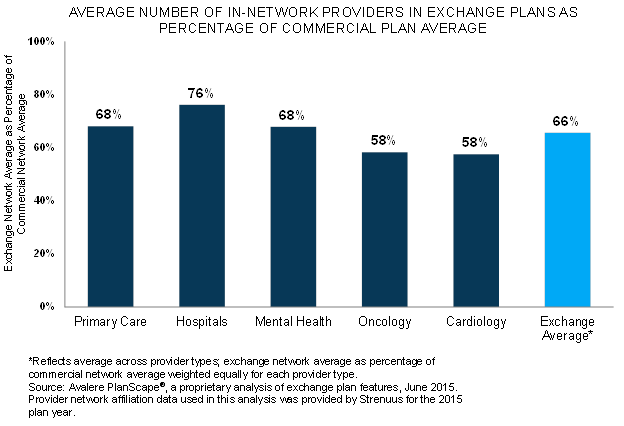
I have posted frequently on the ACA and narrow networks (here and here). How narrow are the networks plans available in the health insurance exchanges? How does provider choice differ between standard commercial insurance plans and those in the exchanges? A study by Avalere finds:
…exchange plan networks include 42 percent fewer oncology and cardiology specialists; 32 percent fewer mental health and primary care providers; and 24 percent fewer hospitals. Importantly, care provided by out-of-network providers does not count toward the out-of-pocket limits put in place by the ACA.
Choice is always a good thing. However, does less choice reduce cost? Likely yes. Does less choice decrease quality? It depends on which providers are included in the network, but the answer is also likely yes. The question is whether any quality decreases are offset by lower premiums through lower reimbursement to these narrower networks of providers. Are patients better or worse off in exchanges? Additional research is needed.