ACOs are all the rage, but what does a typical ACO look like ? A study by Shortell et al. (2014) attempts to answer this question using data from the National Survey of ACOs.
This survey includes ACOs participating in Medicare, Medicaid, or commercial payer programs. The authors consider eight attributes for creating an ACO taxonomy including: “ACO’s size, number of different types of participating provider organizations within the ACO (including nursing or postacute care facilities), the scope of services offered, whether the ACO belongs to an integrated delivery system (IDS), the percent of primary care clinicians, their institutional leadership model, the performance management system used for accountability, and the ACO’s prior experience with payment models other than fee-for-service.”
They classify ACOs into three separate types:
- Larger integrated delivery systems (40%). Largely self-identifying as an integrated delivery system, most of these ACOs are large (mean of 566 FTE physicians) and offer a broad scope of services. About 40 percent of these organizations are physician-led. Further, about 30 percent of ACOs in this category have postacute facilities. “These ACOs have the most experience with payment reform but are relatively lower on their use of performance management/accountability mechanisms.”
- Smaller, physician-led ACOs (34%). These ACOs are physician-lead and are not associated with an IDS. They offer a narrow scope of services, with fewer doctors (mean of 181 FTE physicians) and few include nursing facilities. Most have many PCPs, but little experience with payment reform. They have a high degree of performance management/accountability in place.
- Hybrid ACOs (26%). A hybrid of the two categories above, these groups are of moderate size (mean of 351 FTE physicians) and a moderately large range of services, with about 3 in 10 including post acute services. “They tend to be hospital-led, coalition-led, state/region/county-led, or some other arrangement…” and these entities have some experience with payment reform and relatively low scores on performance management/accountability.
In summary, one should not think of ACOs as a single simplistic entity as this study highlights some of the diversity–as well as some of the commonalities–across ACOs.
The authors also describe relative ACOs performance on cost and quality measures across these three groups.
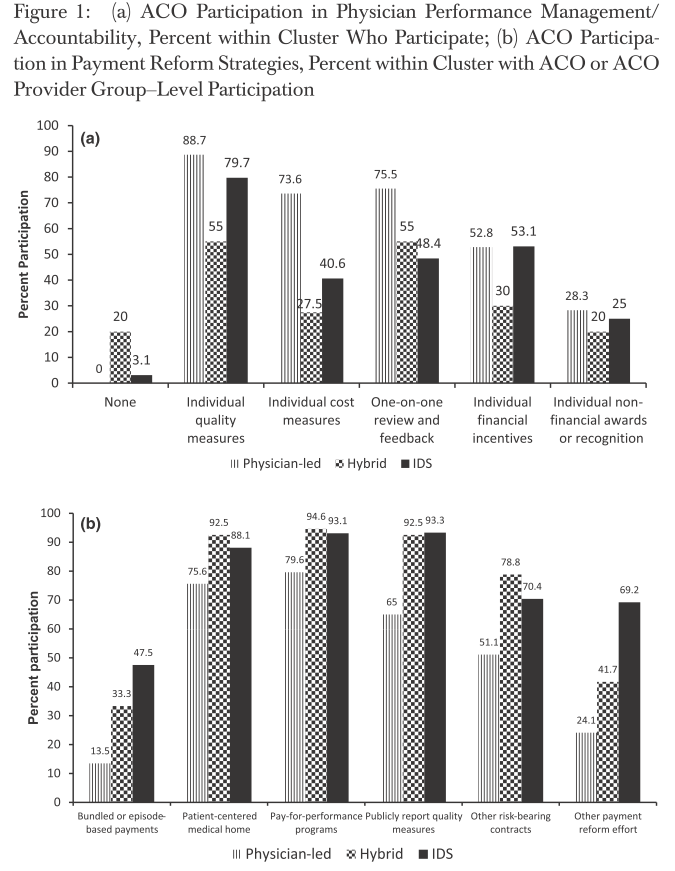
Source:
- Shortell, S. M., Wu, F. M., Lewis, V. A., Colla, C. H. and Fisher, E. S. (2014), A Taxonomy of Accountable Care Organizations for Policy and Practice. Health Services Research. doi: 10.1111/1475-6773.12234
2 Comments