Medicare Advantage has grown over time. In 2020, nearly four in ten (39%) of all Medicare beneficiaries – 24.1 million people out of 62.0 million Medicare beneficiaries overall – were enrolled in Medicare Advantage (MA) plans.
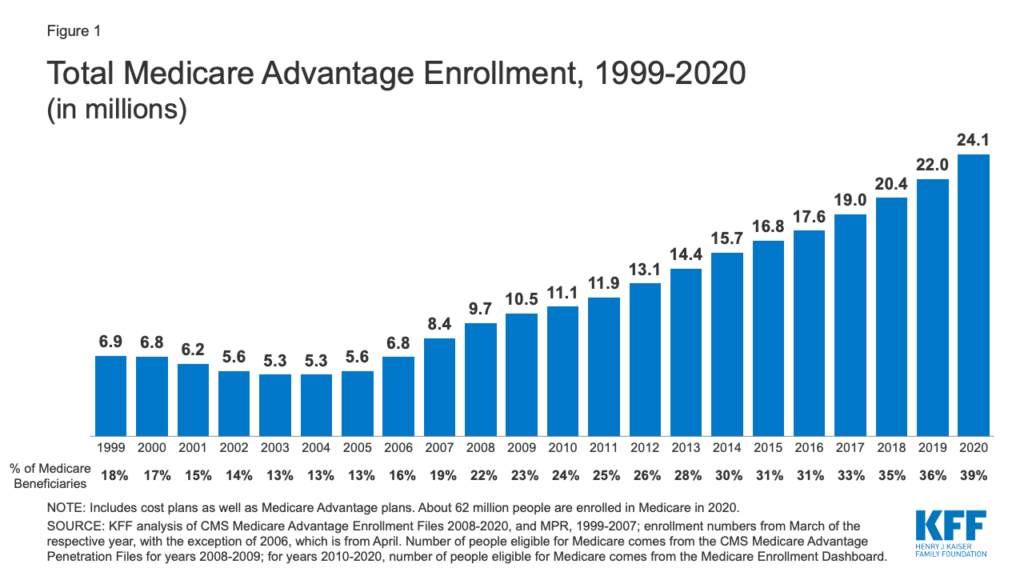
With MA enrollment growing, a key question is who provides higher quality care: Medicare fee-for-service (FFS) or MA? Who is able to better keep cost under control?
To answer this question, a recent paper by Agarwal et al. 2021 conducts a systematic literature review of all studies that use data from 2003 or after. The year 2003 was chosen as that was the year the Medicare Modernization Act was passed. The study excluded Medicare Advantage plans that were limited to Special Needs Plans (SNPs) or those that only included dual-eligible beneficiaries. Based on this literature, the authors identified 48 studies and find that:
…Medicare Advantage was associated with more preventive care visits, fewer hospital admissions and emergency department visits, shorter hospital and skilled nursing facility lengths-of-stay, and lower health care spending. Medicare Advantage outperformed traditional Medicare in most studies comparing quality-of-care metrics. However, the evidence on patient experience, readmission rates, mortality, and racial/ethnic disparities did not show a trend of better performance in Medicare Advantage.
In short, the literature appears to favor Medicare Advantage (MA).
However, there are some concerns with these findings. Healthier individuals may select Medicare Advantage and it is not clear if all included studies were able to adjust for both observable and unobservable health differences between the FFS and MA populations. For instance, Medicare Advantage plans have an incentive to more fully document patient diseases and comorbidities, since CMS’ risk adjustment payments are adjusted for patient health burden. Nevertheless, a systematic review is helpful to understand any quality and cost differences between FFS and MA, particularly as MA enrollment has been growing over time.